
A recent study has turned up something pretty intriguing: in mice with messed-up livers that struggle to clear ammonia, cutting back on dietary protein seems to put the brakes on liver tumor growth.
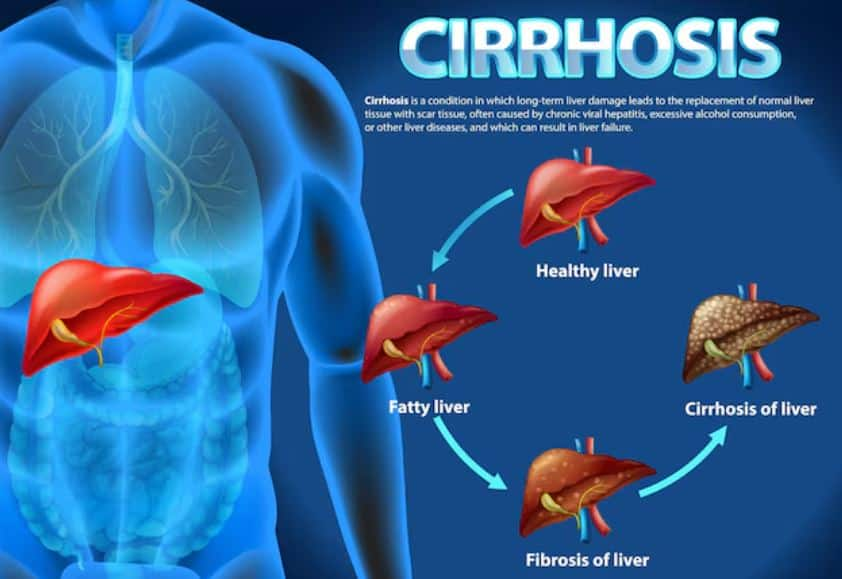
The core idea is surprisingly straightforward. Normally, your liver takes ammonia, a toxic byproduct from breaking down proteins, and converts it safely into urea, which you pee out. But when the liver is damaged (think cirrhosis, fatty liver, chronic hepatitis, or already-present cancer), that cleanup system falters. Ammonia builds up in the liver tissue and blood. And here’s the twist the researchers spotted: tumors appear to hijack that extra ammonia, funneling it into building blocks like amino acids and nucleotides that fuel rapid cell division and DNA synthesis. In other words, what should be waste becomes rocket fuel for the cancer, as reported by Rutgers University (published in Science Advances).
The team, led by Wei-Xing Zong, tested this by giving tumor-prone mice a low-protein diet. Less protein coming in meant less ammonia being produced in the first place. The result? Tumor growth slowed noticeably, and the mice lived significantly longer across different liver cancer models they tried. When they genetically knocked out key enzymes in the ammonia-clearing pathway (the urea cycle), ammonia piled up even more, and sure enough, tumors grew faster and survival dropped. It really points to ammonia overload as a central driver here, not just one random mutation.
They also noticed other perks inside the tumors on the low-protein regimen: less cell proliferation, reduced fibrosis signaling, and dialed-down growth pathways, basically, the cancer cells had a harder time getting the nitrogen they craved for fast multiplication.
Now, before anyone starts slashing protein from their plate, a big caveat: this is not blanket advice for cancer patients. People undergoing treatment often need decent protein to hold onto muscle, stay strong, and recover. Too little can lead to weakness, malnutrition, or worse, especially if you’re already frail. The benefit seems specific to situations where the liver can’t handle normal ammonia loads anymore.
For folks with pre-existing liver issues (alcohol damage, viral hepatitis, NAFLD, etc.), though, the findings raise an interesting question: might carefully monitored lower protein intake become part of managing risk or slowing progression? The researchers themselves are cautious—they stress that mouse results don’t automatically translate to humans. We need proper clinical trials to figure out safe levels, who might benefit most, and how to do this without causing harm.
It serves as a reminder of how metabolism and cancer are interconnected. Something as everyday as protein intake can shift the balance in a damaged liver, turning a normal waste product into something that quietly feeds malignancy. If future human studies hold up, targeting ammonia/nitrogen handling (whether through diet or drugs) could open a new angle for at-risk patients. Worth watching.





















